If you feel a sudden pain in your stomach and wonder whether it’s just gas or something more serious, it could be your appendix. Appendix pain often starts subtly but can quickly turn into a medical emergency if ignored.
Understanding where appendix pain starts, how it moves, and how it feels can help you act quickly. In many cases, early treatment prevents serious complications like rupture or infection.
What does appendix pain feel like?
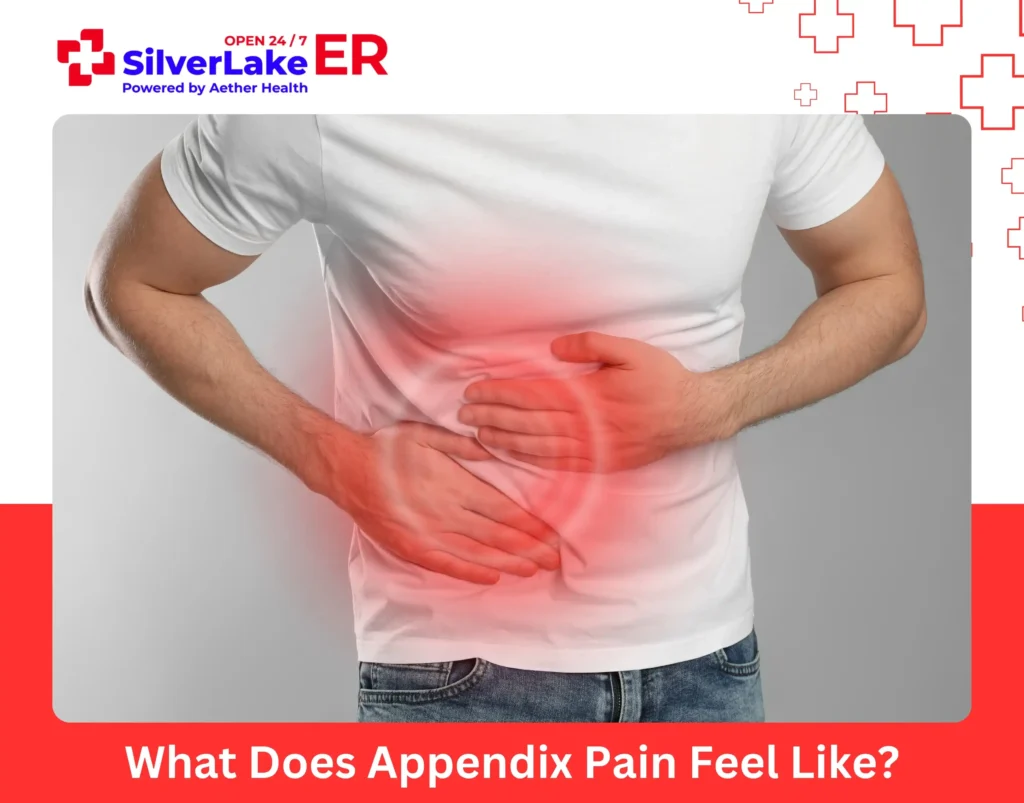
Appendix pain usually starts as a dull ache near the belly button and then moves to the lower right side of the abdomen, where it becomes sharp, constant, and more intense with movement or touch.
Where Does Appendix Pain Start and How Does It Progress?

Appendix pain feels like a dull ache near the belly button that quickly shifts to sharp, constant pain in the lower right abdomen, often worsening with movement or touch. This clear progression makes it different from common stomach discomforts like gas or indigestion.
- Starts near the belly button: Early appendicitis pain often begins as a vague, dull ache around the central abdomen. This happens because the initial irritation is deep inside and not well localized.
- Moves to the lower right side: Within a few hours, the pain tends to shift to the lower right quadrant, where the appendix sits. This migration of pain is considered a hallmark feature of appendicitis.
- Sharp, constant, and worsening: Unlike gas or indigestion, appendix pain doesn’t ease with rest, passing gas, or bowel movements. Instead, it becomes sharper and more constant with time.
- Pain worsens with movement: Walking, coughing, sneezing, or pressing on the area typically makes the pain worse. Many people find themselves hunched over or avoiding sudden movements.
- Tenderness on touch: Applying pressure to the lower right abdomen often elicits strong discomfort, and the pain may intensify when pressure is released (a classic sign called rebound tenderness).
Appendicitis Pain Timeline:
- 0–6 hours: Dull pain near the belly button
- 6–12 hours: Pain shifts to the lower right abdomen
- 12–24 hours: Pain becomes sharp, constant, and more severe
24+ hours: Risk of rupture increases significantly
Other Symptoms That May Accompany Appendix Pain
While pain is the most recognized symptom, appendicitis often comes with additional warning signs:
- Nausea and vomiting that follow the onset of pain
- Loss of appetite (a common early symptom)
- Low grade fever as the body responds to infection
- Bloating or abdominal swelling
- Constipation or diarrhea in some cases
- Difficulty passing gas due to intestinal irritation
These associated symptoms strengthen the likelihood of appendicitis when they appear alongside right sided abdominal pain. Imagine waking up with mild stomach discomfort that feels like indigestion. A few hours later, the pain shifts to your lower right side and becomes sharp and unbearable when you move. This is a classic progression of appendix pain.
How Appendix Pain Differs From Other Abdominal Pain
Abdominal pain can have many causes, but appendicitis has several features that help set it apart:
- Indigestion or gas pain usually comes and goes, improves with bowel movements, or passes on its own.
- Menstrual cramps occur in cycles and are generally lower in the abdomen, often accompanied by other menstrual symptoms.
- Gallbladder pain appears higher in the abdomen, under the right rib cage, and may radiate to the shoulder.
- Kidney stone pain is usually severe and colicky, starting in the flank and moving toward the groin. In contrast, appendix pain is progressive, steady, and moves from the belly button to the lower right abdomen. It does not resolve without treatment.
Appendicitis vs Other Abdominal Pain
- Gas pain: Comes and goes and often improves after passing gas
- Appendix pain: Gets worse over time and does not improve
- Kidney stones: Severe, wave-like pain moving from back to groin
- Gallbladder pain: Upper right abdomen, often after fatty meals
Who Is Most at Risk of Appendicitis?
Appendicitis can occur in anyone, but certain groups are more commonly affected:
- Children and teenagers between 10–19 years old are at the highest risk.
- Young adults up to age 30 are also commonly diagnosed.
- Men are slightly more likely to experience appendicitis than women.
- People with a family history of appendicitis may also be at greater risk.
When to Seek Emergency Care for Appendix Pain
Appendicitis is a medical emergency. You should seek immediate care if you notice:
- Severe, persistent abdominal pain that starts near the navel and shifts to the lower right side
- Pain that worsens with movement, coughing, or pressing on the abdomen
- Pain accompanied by fever, nausea, or vomiting
- Abdominal swelling or bloating that increases over time
A ruptured appendix can cause peritonitis, a life threatening infection that spreads throughout the abdominal cavity. This is why prompt diagnosis and surgery are essential.
Diagnosis of Appendicitis
Doctors use a combination of physical exams, blood tests, and imaging to diagnose appendicitis:
- Physical exam: Checking for tenderness, rebound pain, and guarding.
- Blood tests: Elevated white blood cell count can signal infection.
- Urine tests: To rule out urinary tract infections or kidney stones.
- Imaging: Ultrasound, CT scans, or MRI can confirm inflammation and guide treatment.
What Happens at the ER for Appendix Pain?
When you visit the emergency room with suspected appendicitis, doctors will:
- Perform a physical examination to check for tenderness and rebound pain
- Order blood tests to detect infection
- Use imaging tests like a CT scan or ultrasound to confirm diagnosis
- Prepare for immediate surgery if appendicitis is confirmed
Most patients are diagnosed within a few hours and treated promptly to avoid complications.
Treatment for Appendix Pain

The standard treatment for appendicitis is surgical removal of the appendix (appendectomy). This can be done through:
- Laparoscopic surgery: Minimally invasive and usually involves quicker recovery.
- Open surgery: Sometimes necessary in complicated or ruptured cases.
In some cases of uncomplicated appendicitis, antibiotics may be used initially, but surgery remains the most definitive treatment.
Recovery After Appendectomy
Recovery times depend on the type of surgery and whether the appendix ruptured:
- Laparoscopic surgery: Most people return to light activity within a week.
- Open surgery: Full recovery may take 4–6 weeks.
- Ruptured appendix: Longer hospital stay, antibiotics, and more cautious recovery.
Following your surgeon’s instructions about rest, wound care, and physical activity is key to smooth recovery.
Preventive Insights
There is no guaranteed way to prevent appendicitis, but some factors may lower risks:
- A diet high in fiber may support digestive health.
- Staying hydrated helps reduce constipation and intestinal blockages.
- Seeking early care for unexplained abdominal pain prevents delayed treatment.
Key Takeaway
Appendix pain should never be ignored. If your pain starts near the belly button and moves to the lower right side, especially with nausea or fever, seek medical care immediately. Early diagnosis and treatment can prevent rupture and ensure a faster, safer recovery.
Frequently Asked Questions (FAQs)
Where exactly is appendix pain located?
Appendix pain usually starts near the belly button and then moves to the lower right side of the abdomen.
How do I know if it’s gas or appendicitis?
Gas pain comes and goes and improves, while appendix pain steadily worsens and does not go away.
Does appendix pain come and go?
No, it typically becomes constant and more severe over time.
How fast does appendicitis get worse?
Symptoms usually worsen within 12–24 hours.
When should I go to the ER for appendix pain?
If pain is severe, worsening, or accompanied by fever, nausea, or vomiting, seek immediate medical care.