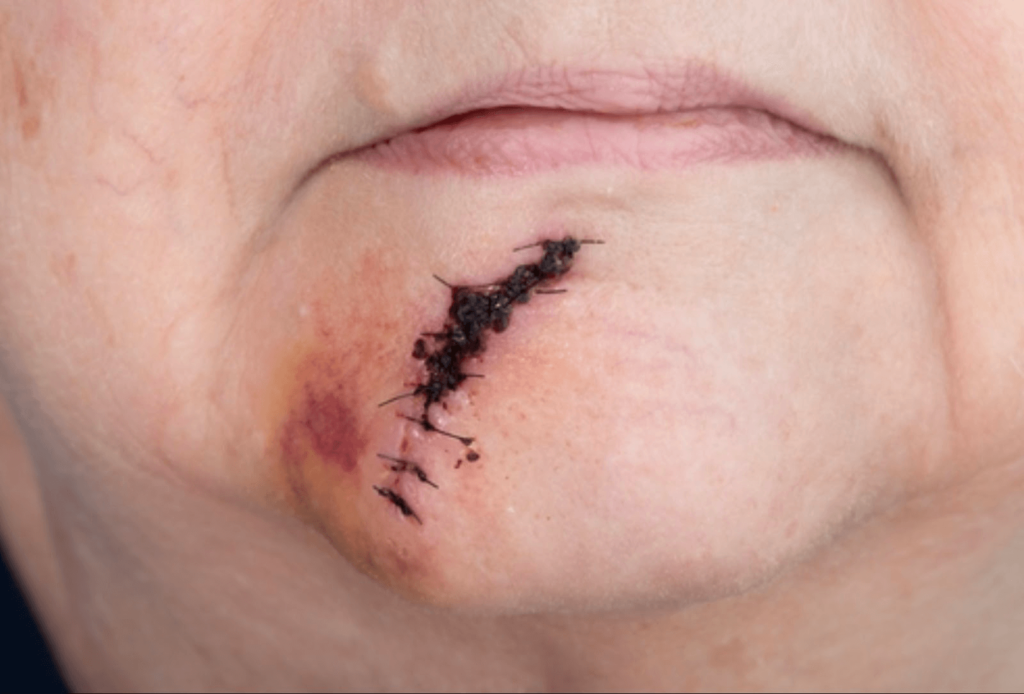
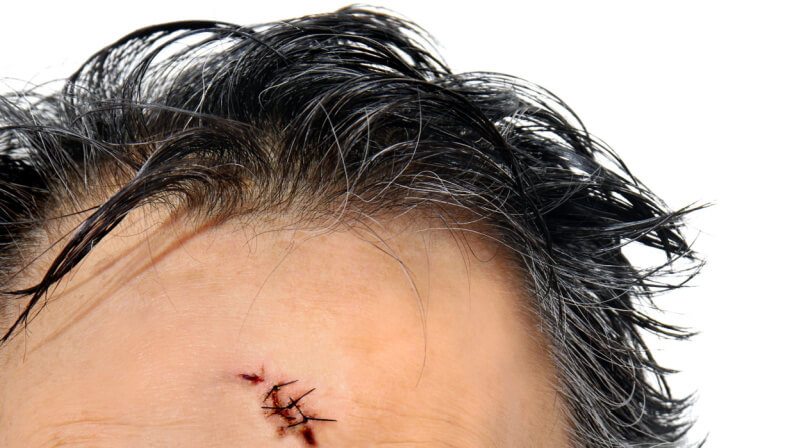
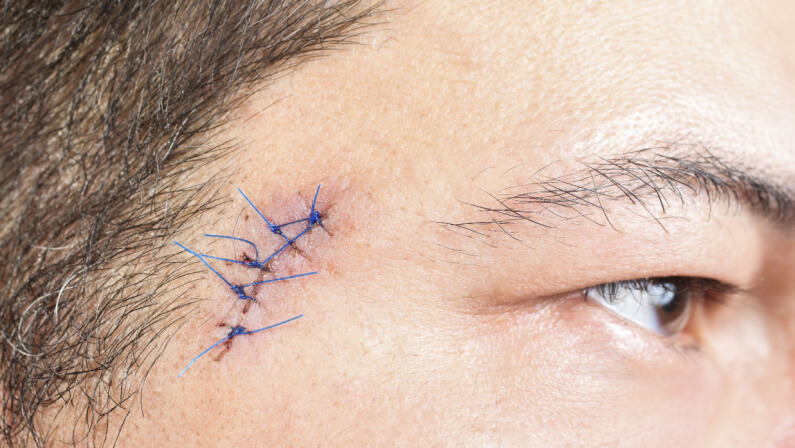
Imagine facing an unexpected accident that results in a facial laceration, leaving both a physical and emotional mark. In such moments, understanding the comprehensive process of facial laceration repair becomes crucial.
Facial laceration repair involves more than simply stitching up the wound; it requires meticulous techniques that prioritize both functionality and aesthetics. This guide provides a thorough exploration of facial laceration repair, ranging from understanding types and assessing severity to the intricacies of the repair process and potential complications.
What Are Facial Lacerations and How Do They Occur?
Facial lacerations are cuts or tears in the skin of the face, often caused by trauma or injury. They can vary in severity, from minor cuts that only affect the top layer of skin to more extensive injuries that involve deeper tissues, such as muscles, blood vessels, and nerves. These kinds of lacerations can come about from various situations, such as accidents, falls, sports mishaps, physical altercations, and even surgical procedures.
The seriousness of a facial laceration depends on things like how deep, how long, and where the cut is. Minor lacerations might only need basic care for the wound, but if the cut is deeper or more complicated, it might need medical attention, like stitches or sutures.
When Is Facial Laceration Repair Necessary?
Facial laceration repair becomes necessary when there are cuts or tears on the skin of the face that require medical attention for proper healing and cosmetic outcomes. The need for repair is determined by the severity and characteristics of the laceration.
Here are some scenarios when facial laceration repair is necessary:
Depth and Extent
If the laceration goes beyond the superficial layer of the skin and involves deeper tissues, such as muscles, blood vessels, or nerves, it is likely to require repair.
Bleeding
If the laceration is causing significant bleeding that doesn’t stop with simple pressure, medical attention is necessary to control bleeding and prevent complications.
Cosmetic Concerns
Lacerations on the face may lead to noticeable scars if not repaired properly. To minimize scarring and maintain the best cosmetic appearance, repair by a medical professional might be recommended.
Functional Impairment
Lacerations that affect the function of facial muscles, nerves, or structures like the eyelids or lips can require repair to restore proper function.
Risk of Infection
Deep or jagged lacerations have a higher risk of infection. Medical professionals may recommend repair to reduce the risk and ensure proper wound healing.
Wound Closure
Some lacerations are too wide or deep to heal properly on their own. Sutures, stitches, or adhesive strips might be needed to hold the edges of the wound together for optimal healing.
Location
Lacerations in certain areas of the face, such as around the eyes, nose, or mouth, are more likely to need repair due to the potential for functional or cosmetic complications.
Childhood Injuries
In cases involving children, facial lacerations are often repaired to minimize scarring as children’s skin tends to heal differently compared to adults.
Ultimately, the decision for facial laceration repair is made by a medical professional based on careful evaluation of the wound’s characteristics, potential complications, and the desired cosmetic and functional outcomes. Seeking timely medical attention for facial lacerations is important to ensure proper healing, reduce the risk of complications, and achieve the best possible results.
Different Types of Facial Lacerations
Facial lacerations are not homogenous; they vary in depth, length, and complexity. They can be categorized based on location, tissue involvement, and potential effects on underlying structures. Understanding these helps medical professionals make informed decisions regarding treatment strategies.
Simple Lacerations
These are relatively uncomplicated wounds that are confined to the surface layer of the skin. Simple lacerations are typically superficial and often require straightforward wound care, such as cleansing and dressing.
Complex Lacerations
In contrast, complex lacerations extend beyond the superficial layer, making their way into deeper tissue levels. These wounds can traverse through layers of muscle, fat, and in some instances, even reach down to the bone. Repairing complex lacerations may involve a more intricate approach to ensure proper healing and cosmetic restoration.
Lacerations Proximate to Vital Structures
Certain lacerations are strategically positioned near crucial anatomical elements like nerves, blood vessels, and sensory organs. Injuries in these regions can have more significant implications, potentially affecting functionality or leading to heightened risks. Precise evaluation and meticulous repair techniques are often necessary to mitigate potential complications and promote optimal recovery.
How Is Facial Laceration Severity Assessed?
The process of evaluating the severity of facial lacerations involves a systematic approach to determine the extent of the injury and guide appropriate treatment decisions.
Here’s an overview of how facial laceration severity is assessed:
- Depth Examination: The depth of the laceration is carefully evaluated to ascertain whether it is confined to the skin’s surface or extends into deeper layers of tissue, such as muscle, fat, or bone.
- Length Analysis: The length of the laceration is measured, providing insight into the extent of the injury and its potential impact on surrounding structures.
- Length Measurement: The length of the laceration is measured to gauge the overall size of the wound. This measurement provides valuable information about the extent of tissue damage and potential complications.
- Location Analysis: The specific location of the laceration on the face is considered. Lacerations near vital structures such as blood vessels, nerves, or sensitive areas can have different implications and may require specialized attention.
- Evaluation of Underlying Structures: Medical professionals assess whether the laceration affects underlying anatomical structures like muscles or bones. Injuries involving these structures can impact functionality and require specific approaches to repair.
- Cosmetic Impact: The potential cosmetic impact of the laceration is taken into account. Lacerations on the face can result in visible scars, so assessing the potential for scarring helps determine the optimal repair technique.
- Bleeding and Tissue Loss: The amount of bleeding and tissue loss caused by the laceration is evaluated. Excessive bleeding or tissue loss can indicate a more severe injury.
- Patient’s Medical History: The patient’s medical history, including any pre-existing conditions or medications, is considered, as it can influence wound healing and treatment options.
What Is the Facial Laceration Repair Process?
The procedure for addressing facial lacerations involves a structured series of actions aimed at effectively treating cuts and tears on the face.
Here’s a simplified overview of how this process goes:
- Initial Assessment: Medical professionals begin by closely examining the laceration’s characteristics, including its depth, length, location, and potential involvement of underlying structures. This assessment forms the basis for a tailored treatment plan.
- Anesthesia Administration: Local anesthesia is skillfully administered to ensure patient comfort by numbing the area surrounding the laceration before repair procedures commence.
- Cleaning and Preparation: Prior to repair, the immediate vicinity of the laceration is meticulously cleansed and sterilized to mitigate the risk of infection. Debris and foreign particles are cautiously removed from the wound area.
- Tissue Realignment: For lacerations with irregular or jagged edges, meticulous alignment of the wound edges takes place to facilitate optimal closure. This precision promotes superior healing outcomes and minimizes scar formation.
- Closure Technique: The appropriate closure method is chosen based on the specific characteristics of the laceration. Options include adhesive strips, skin glue, sutures, or stitches, tailored to the wound’s complexity.
- Layered Closure (If Necessary): Deeper lacerations that traverse multiple tissue layers may require a layered closure approach to ensure thorough repair and optimal healing conditions.
- Dressing Application: A sterile dressing is expertly applied over the repaired laceration to provide a barrier against external contaminants, fostering an environment conducive to healing.
- Post-Procedure Care: Patients are provided with comprehensive instructions for wound care during the healing process. This encompasses guidance on maintaining cleanliness, avoiding certain activities, and managing potential discomfort.
- Follow-up Appointments: Depending on the laceration’s nature, patients are scheduled for follow-up appointments to monitor the progress of healing. This allows for the timely removal of any sutures or stitches if required.
- Consideration for Aesthetic Outcomes: In cases where the laceration’s location might impact aesthetics, efforts are made to minimize scarring and ensure optimal cosmetic results.
What Are the Different Techniques for Facial Laceration Repair?
Repair techniques vary based on wound characteristics such as location, severity, and cosmetic considerations.
Common approaches include:
Adhesive Strips or Steri-Strips
Minor lacerations can often be managed using adhesive strips that hold the wound edges together. These strips are applied directly over the wound and create a temporary bond while the skin heals naturally.
Skin Glue (Dermabond)
Skin glue , or Dermabond, is a medical adhesive that is applied to the wound to hold the edges together. It forms a protective barrier and falls off on its own as the wound heals beneath.
Sutures (Stitches)
Suturing involves using medical threads to stitch the wound edges together. Different suture techniques, such as simple interrupted, running, or buried stitches, may be used depending on the laceration’s complexity.
Absorbable Sutures
In some cases, absorbable sutures are used, which are naturally broken down by the body over time and do not require removal.
Non-Absorbable Sutures
Non-absorbable sutures need to be removed by a medical professional after the wound heals.
Deep Sutures
For deeper lacerations that involve multiple tissue layers, deep sutures are used to close the underlying layers, providing additional support.
Subcuticular Sutures
These sutures are placed beneath the skin’s surface and are not visible externally, reducing the potential for scarring.
Staples
Staples are metal clips that can be used to close larger or longer lacerations. They are quick to apply and remove.
Injectable Tissue Adhesives
Certain medical adhesives can be injected beneath the skin’s surface to provide internal support and aid in wound closure.
Specialized Techniques
In cases of complex or intricate lacerations, specialized techniques may be employed. This could involve plastic surgery methods to ensure optimal healing and cosmetic results.
Does Facial Laceration Repair Impact Cosmetic Outcomes?
Facial lacerations, particularly those situated in prominent areas, can lead to visible scars that impact a person’s appearance. The approach taken during facial laceration repair plays a pivotal role in determining the eventual cosmetic result.
Factors affecting cosmetic outcomes include:
- Repair Technique: The choice of sutures, adhesive strips, or skin glue significantly influences scarring and healing.
- Laceration Location: Areas with high tension, like around the eyes or lips, require special attention to minimize tension and ensure better cosmetic outcomes.
- Medical Professional’s Expertise: Accurate wound alignment and closure by skilled professionals contribute to improved cosmetic results.
- Wound Care Practices: Patient compliance with post-repair wound care instructions influences scar formation and healing.
- Individual Healing Response: Genetic factors, age, and overall health influence how well scars form.
Open communication between the patient and healthcare provider is vital. Patient concerns about potential scarring enable healthcare professionals to set realistic expectations and offer tailored recommendations.
Can Facial Lacerations Affect Nerves and Blood Vessels?
Facial lacerations can harm vital nerves and blood vessels due to their close proximity. The face houses intricate networks of these structures.
When a laceration occurs, these can be damaged, leading to complications:
Blood Vessels
The face has a rich blood supply due to the many blood vessels that run through it. If a laceration cuts through or damages these vessels, it can lead to bleeding. In some cases, the bleeding might be minor and stop on its own, but in more severe cases, it could be significant and require medical intervention to stop the bleeding.
Nerves
Nerves in the face control movement, sensation, and expression. If a facial laceration damages these nerves, it can result in loss of sensation, difficulty moving certain facial muscles, or even paralysis in extreme cases. Nerve damage can lead to long-lasting functional and cosmetic issues, as nerves may need time to heal and regenerate, and in some cases, they might not fully recover.
How Is Pain Managed During and After Facial Laceration Repair?
Pain management during and after facial laceration repair involves a combination of strategies to ensure the patient’s comfort and minimize discomfort during the procedure and the recovery period.
Here are some common approaches:
Local Anesthesia
Local anesthesia is administered before the repair procedure. This numbs the area around the laceration, ensuring that the patient does not feel pain during the repair. Anesthesia can be delivered through injections or topical applications.
Anesthetic Creams or Gels
Anesthetic creams or gels may be applied to the skin before the procedure. These products numb the surface of the skin, making the injections for local anesthesia more comfortable.
Nerve Blocks
For more extensive repairs or deeper lacerations, nerve blocks can be used. Numbing medication is injected near larger nerves to provide comprehensive pain relief for the entire area being treated.
During the Procedure
Throughout the repair process, patients should feel minimal to no pain due to the effect of the administered local anesthesia. Any sensations they experience should be limited to pressure or movement.
Post-Procedure Pain Management
After the procedure, patients might experience mild discomfort, swelling, or soreness. Pain relievers such as over-the-counter non-prescription pain medications (e.g., acetaminophen or ibuprofen) are often recommended to manage this discomfort.
Prescription Pain Medications
In cases of more significant discomfort, prescription pain medications may be prescribed by the healthcare provider. These medications are tailored to the patient’s needs and should be taken as directed.
Cold Compresses
Applying cold compresses to the treated area can help reduce swelling and provide relief from any residual pain or discomfort.
Follow-Up Care
Proper wound care can also contribute to pain management. Keeping the wound clean, following any instructions provided by the healthcare provider, and avoiding activities that could disrupt the healing process can help prevent unnecessary discomfort.
Psychological Support
It’s important to address any psychological distress the patient might experience, especially if the laceration was a result of a traumatic event. Providing emotional support and addressing anxiety can indirectly contribute to pain management.
Remember that pain is subjective, and everyone’s pain tolerance is different. It’s essential to communicate openly with your healthcare provider about your comfort level and any pain you might be experiencing so that they can adjust their approach accordingly.
Is Follow-Up Care Necessary After Facial Laceration Repair?
After getting your facial laceration repaired, it’s important to have follow-up appointments with your healthcare provider . These appointments help make sure that your wound is healing the right way and that you’re getting the best results possible.
During these follow-up visits, your healthcare provider will check how your wound is doing. They’ll look for any signs of infection, like redness or swelling, and make sure that your skin is healing well. If your wound was closed with stitches, they’ll also take those out at the right time to help your skin heal properly.
If you’re worried about anything during your healing process, these appointments are a good time to ask questions and get the right answers.
What Are the Potential Complications of Facial Lacerations?
Facial lacerations, while common, can lead to various complications due to the intricate nature of the face and its underlying structures.
Here’s an overview of potential complications associated with facial lacerations:
Infection
Facial lacerations can provide a route for bacteria to enter the body. Infection risk is heightened due to the face’s exposure to the environment. Signs of infection include increased redness, swelling, warmth, pus, and fever.
Scarring
Even with proper wound closure, scarring is a common concern. Factors such as the wound’s depth, location, and individual healing response influence scar formation. Skillful repair techniques can help minimize visible scarring.
Nerve and Blood Vessel Damage
Lacerations near nerves and blood vessels can lead to functional issues, altered sensations, or bleeding. Nerve damage might result in loss of muscle control or unusual sensations like tingling.
Tissue Necrosis
In some cases, the blood supply to a repaired laceration may be compromised, leading to tissue death (necrosis). This can result in delayed wound healing or even require corrective interventions.
Dehiscence
Wound dehiscence occurs when the wound edges separate after closure. This can expose underlying tissue and increase the risk of infection. Dehiscence is more likely in wounds under tension.
Hematoma
Blood vessels damaged during a laceration repair can lead to the accumulation of blood under the skin, causing swelling and discomfort known as a hematoma.
Hypertrophic or Keloid Scars
In some cases, scars can become raised, thickened, or extend beyond the original wound site. These are known as hypertrophic or keloid scars and might require additional treatment.
Functional Impairment
Depending on the laceration’s location and severity, facial movements, expressions, or sensory functions might be affected, leading to temporary or permanent functional impairment.
Aesthetic Concerns
Unsatisfactory cosmetic outcomes, including asymmetry or visible scarring, can lead to aesthetic dissatisfaction.
Expert Care at Aether Health – SilverLake ER in Pearland, TX
Facial laceration repair demands expertise, precision, and a commitment to both function and aesthetics. If you’re seeking top-tier care in Pearland, TX, visit Aether Health – SilverLake ER . Our experienced medical team, advanced facilities, and patient-centric approach ensure optimal recovery and peace of mind for your facial laceration repair procedure.
Contact Aether Health – SilverLake ER today to experience the transformative impact of meticulous facial laceration repair guided by professionals who prioritize your well-being.